From this article you will learn:
- what causes gingivitis,
- what are the forms of this disease,
- gingivitis in adults - symptoms and treatment at the dentist.
The article was written by a dentist with more than 19 years of experience.
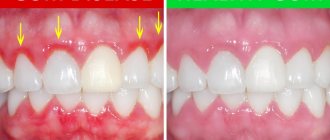
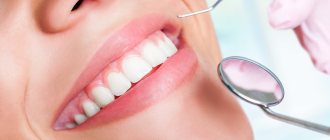
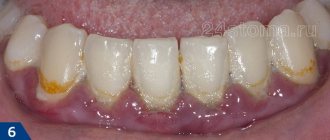
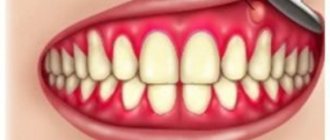
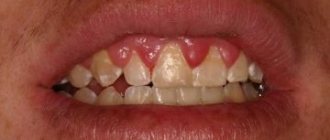
Gingivitis is an inflammation of the marginal part of the gum adjacent to the teeth, including the interdental papillae (Fig. 1-2). With this disease, patients most often complain of bleeding gums, pain when brushing teeth, as well as swelling, redness or cyanosis of the gums. Gingivitis with a predominance of such symptoms is usually called “catarrhal” by dentists.
However, in a small percentage of cases, inflammation can also manifest as gingival overgrowth, or even ulceration and necrosis. The most important feature that distinguishes gingivitis from other inflammatory gum diseases is that the inflammation does not spread deeper than the gum mucosa. Accordingly, with gingivitis there is no destruction of the bone tissue around the teeth, no mobility of the teeth, i.e. symptoms of a disease such as periodontitis.
Gingivitis: photo, diagram
If you have mobility of some teeth, as well as periodontal pockets, from which pus can be released during periods of exacerbation, such symptoms no longer indicate gingivitis, but the presence of periodontitis (a more severe form of gum inflammation). You can read more about this disease at the link above. Let us only note that in most cases the development of periodontitis is a consequence of untimely and/or ineffective treatment of gingivitis.
Main forms of gingivitis:
- catarrhal gingivitis (Fig. 1-8),
- ulcerative-necrotizing gingivitis (Fig. 12-15),
- hypertrophic gingivitis (Fig. 16-18).
In this article we will analyze in detail each form of gingivitis, indicating effective drugs and regimens for their use. We will also list patients’ mistakes in the process of self-medication, which often lead to the development of severe chronic gum inflammation. If you are more interested in how to properly treat gingivitis not in adults, but in children, then read more about this in the article: → Gingivitis - symptoms and treatment in children
Causes of gingivitis
The most common cause of gingivitis is poor personal oral hygiene. Violation of the rules may consist of inappropriate technique, irregular brushing of teeth, refusal to use dental floss and rinses after meals. As a result, food particles accumulate between the teeth, and a large amount of soft plaque forms on the surface of the teeth. This is a favorable environment for the proliferation of bacteria, which leads to the inflammatory process.
Soft plaque, which is not removed for a long time, mineralizes and hardens over time. When tartar appears, pathogenic microorganisms also actively multiply on it. In addition, the sharp edges of hard deposits injure the gum margin, which reduces local protective factors.
There are other common local causes of gingivitis:
- unsound orthopedic, orthodontic structures: braces with sharp edges,
- chips of enamel, destruction of teeth and fillings: injury to mucous membranes with sharp edges;
- teething disorders, dental caries, pulpitis, periodontitis, abscesses and other diseases;
Systemic pathologies and certain conditions can lead to the development of gum inflammation. The most common ones are:
- endocrine diseases - diabetes mellitus, Graves' disease, etc.;
- diseases of the digestive system - gastroesophageal reflux, Crohn's disease, chronic cholecystitis, etc.;
- hypovitaminosis, lack of minerals due to a strict diet or impaired absorption of nutrients;
- taking certain medications - antidepressants, local vasoconstrictors, antibiotics, combined contraceptives, beta-blockers, etc.;
- past infections and surgical interventions;
- puberty, pregnancy, menopause - changes in hormonal status not associated with illness;
- allergic reactions to food, medicines, hygiene products;
- bad habits.
Often there is a combination of factors - a combination of local and general causes of weakening of immune forces. You can find out the exact reasons only with the help of a doctor.
Ask a Question
Juvenile gingivitis
Juvenile gingivitis has a second name – juvenile. Juvenile gingivitis develops during puberty, during puberty. Typically, gum inflammation is observed in girls 1-2 years before the appearance of the first menstruation, and in boys - at 14-15 years. As a rule, after one or two years it goes away without a trace, but sometimes it can turn into a hypertrophic form.
What are the signs of juvenile gingivitis? The intergingival papillae become bright red, swollen and painful. As teeth become difficult to care for, plaque accumulates and turns into tartar, which in turn irritates the gums even more. Typically, juvenile gingivitis affects the gums in the area of the front teeth.
Symptoms and consequences
Symptoms of gingivitis are determined by stage. The disease can begin with the following manifestations:
- swelling, redness, looseness of the gums;
- increased sensitivity of tissues, bleeding during brushing teeth and eating due to fragility of blood vessels;
- pain when chewing and touching;
- bad breath.
As the disease progresses, the necks of the teeth may become exposed, which leads to increased sensitivity of the teeth - it becomes difficult to accept hot and cold drinks and foods. The pain also increases over time, and severe difficulty chewing food may occur. In addition to general symptoms, there are also specific ones characteristic of a particular type of gingivitis.
The consequences of gum inflammation can be very serious: the pathological process often spreads to the ligamentous apparatus of the tooth, and periodontitis occurs. This condition is dangerous due to the mobility of teeth and the high probability of their loss. A chronic focus of inflammation in the mouth is a risk factor for the development of diseases of the ENT organs.
Effective pharmaceutical preparations and traditional medicine: we treat gums that are inflamed
If you notice the slightest signs of inflammation in your gums, you should immediately consult a doctor. Such diseases develop very quickly, and the sooner you begin adequate treatment, the easier it will be to stop the pathological process, avoiding complications. Here you need to understand that only a specialized specialist – a periodontist – can select effective treatment tactics. Home methods are permissible only as part of maintenance therapy and only if agreed with the doctor. Read further in the article about how to treat inflamed gums in adults and children.
Types of gingivitis
Gingivitis can be acute or chronic. In the first case, noticeable symptoms occur. Chronic forms are characterized by mild symptoms, pain is absent or minimal. Periodic slight bleeding of the gums during brushing and halitosis may occur. It is important to understand that sluggish gingivitis is characterized by periodic exacerbations.
Inflammation of the gums is classified not only by its form, but also by the nature of its course.
Catarrhal gingivitis
Catarrhal gingivitis is characterized by redness of the gum area. Itching and bleeding due to mechanical action and mild pain may occur. This is the most common and easiest to treat type of inflammation. Quite often it acts as the initial stage of development of other forms.
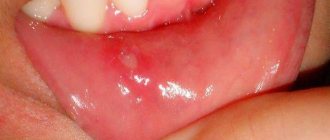
Ulcerative gingivitis
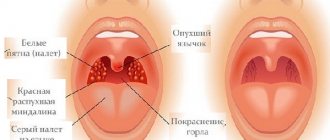
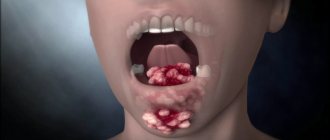
Necrotizing ulcerative gingivitis is characterized by the formation of open ulcers, death of areas of gum tissue, and strong bad breath. One of the typical symptoms is the appearance of a grayish coating. The disease is more difficult to treat; in the absence of timely assistance, purulent foci and severe necrosis may appear.
Hypertrophic and atrophic gingivitis
Ulcerative-necrotic gingivitis is followed by hypertrophic gingivitis - excessive growth of tissues occurs that cover the crowns of the teeth. There is keratinization of areas of the gums.
The atrophic form of the disease, on the contrary, is characterized by a decrease in the level of the gums and exposure of the necks of the teeth. This condition is dangerous due to the loss of healthy teeth.
Desquamative gingivitis
This type of inflammation is characterized by abundant desquamation of the gum epithelium. Distinctive features are pronounced redness and noticeable peeling areas of the surface of the mucous membranes.
Diagnostic features
Gingivitis can be recognized visually—sometimes one examination by a doctor is enough. But you should make sure that there are no more serious pathologies, so diagnosis may include not only a visual assessment of the condition of the oral cavity, but also other measures:
- collecting anamnesis, assessing the condition of structures in the oral cavity;
- probing of periodontal pockets if present;
- determination of tooth mobility;
- electroodontodiagnosis to determine the condition of the dental pulp;
- panoramic x-ray or targeted x-ray - to exclude periodontitis, periostitis and other pathologies of deep structures, jaw bone tissue, etc.
It is important to take into account the presence of chronic diseases and medications. Only with complete information can a doctor make an accurate diagnosis and develop an effective treatment regimen.
Medicines in tablet form
As part of the treatment of inflammatory diseases, doctors often prescribe oral medications. These may be antibiotics, which are necessarily prescribed when purulent processes occur. Antihistamines, immunostimulants, and multivitamin complexes are also used.
Antibiotics to combat the proliferation of pathogenic bacteria
To stop the proliferation of pathogenic bacteria, doctors prescribe additional antibacterial drugs for oral administration. It is antibiotics that are necessarily prescribed when the discharge of pus begins. These drugs are potent drugs, so they can only be taken as prescribed by a specialist. In dentistry, Lincomycin, Glycosamil and Clindamycin are often used.
To stop the proliferation of pathogenic bacteria, doctors prescribe antibiotics
Antihistamines and immune boosters
Antihistamines are usually prescribed in combination with antibiotics to prevent allergic reactions. This could be Tavegil, Diazolin or Fenistil. To increase the body's immune forces, Ribomunil or Imudon are prescribed.
Multivitamin complexes
Multivitamin complexes are also used as maintenance therapy. To stimulate the healing of wounds and damaged tissues, vitamin C and retinol are recommended in particular.
Principles of treatment
Treatment of gingivitis begins with hygiene: professional teeth cleaning. It is important to remove soft and hard dental plaque. For this, hand tools, an ultrasonic scaler, and the powder blasting method can be used. Subgingival dental plaque can be removed using the Vector device.
It is important to eliminate foci of infection - to fill teeth affected by caries, to undergo endodontic treatment in the presence of pulpitis, to remove the roots of teeth that cannot be restored and are not involved in the prosthetic process.
It is necessary not only to pay attention to the causes of the disease, but also to reduce the influence of harmful factors:
- stop smoking;
- consume food and drinks only at a comfortable temperature;
- remove spicy and smoked foods, marinades, especially those with vinegar, from the diet;
- During the treatment period, try to eat less solid food so as not to injure the loose gum tissue.
If the source of injury to the mucous membrane is the sharp edges of teeth or dentures, the doctor will immediately take measures to prevent further damage or recommend contacting a dentist of another profile - an orthopedist, an orthodontist.
Drugs for the treatment of gingivitis
Treatment for gingivitis may involve the use of medications in different forms. Mouth rinses based on antiseptics allow you to solve two problems at once: mechanically remove food debris and bacterial plaque, and also deliver active ingredients to inflamed tissues. Dentists recommend using ready-made pharmaceutical products; in each specific case, a specialist will prescribe a medicinal solution to quickly alleviate the condition. Ready-made formulations are more convenient to use, and the concentration of active components in them is known, this distinguishes them from traditional methods.
The most popular are rinses based on the following antiseptics:
- chlorhexidine;
- furacillin;
- chlorophyllipt;
- Metronidazole.
Calendula, chamomile, yarrow, oak bark, and St. John's wort have antiseptic properties. Doctors do not recommend preparing alcohol infusions; it is better to choose decoctions. The recipes call for using one teaspoon of dry raw materials per glass of boiling water. It is important to cool the broth to a comfortable temperature. Take into account possible allergic reactions, give preference to those herbs to which there was no previous intolerance. It is necessary to discuss with your doctor the possibility of using traditional methods.
Effective drugs for the treatment of gingivitis are ointments and gels. Multicomponent local products for applications not only help relieve inflammation, but also have an analgesic, decongestant, and antipruritic effect. The active components of such drugs can be lidocaine, antibacterial, antifungal substances, and antiseptics. The doctor will select a gel or ointment taking into account the shape and type of gingivitis. Thus, for ulcerative inflammation, it may be advisable to use regenerating agents, and acute catarrhal gingivitis will require the use of a powerful anesthetic gel.
For hypertrophic gingivitis, surgery may be required - a simple gingivectomy. This operation involves excision of excess tissue and application of a bandage, and is performed under local anesthesia.
How to rinse your mouth to relieve inflammation
Rinsing with antibacterial and anti-inflammatory solutions is a mandatory step in treatment. Moreover, it is allowed to use both pharmaceutical drugs and those prepared independently from medicinal plants. You need to understand that rinsing is part of symptomatic therapy. This is not a primary treatment, but it helps relieve acute symptoms and stimulate the healing process of damaged tissue. Therefore, the use of any solutions is allowed only as prescribed by a doctor.
Pharmacy drugs
When answering the question of how you can treat inflamed tissues in the oral cavity, first of all you need to pay attention to the appropriate rinses. Almost all of them combine antiseptic, analgesic and anti-inflammatory properties. For example, in case of inflammation of the mucous membrane, including when it moves away from the tooth and accumulation of deposits under the crown (in periodontal pockets), doctors usually prescribe the following medications:
- "Chlorhexidine" - use for rinsing after each meal,
- "Furacilin" - 2-3 times a day,
- "Miramistin" - up to 3-4 times a day,
- "Chlorophyllipt" - requires preliminary dilution, after which the product can be used up to 3 times a day.
In some cases, Miramistin is prescribed
“Chlorhexidine and soda-saline solution always help me. The latter is absolutely super - the simplest but most effective remedy, it has never failed! And I’ve been suffering with gingivitis for a long time. The main thing that is needed is to quickly begin treatment during an exacerbation, then the symptoms will go away immediately. Well, for good measure, of course, you definitely need to go to a periodontist. I go for cleaning every six months. For those who have problem gums, this is a mandatory procedure and should not be skipped.”
Nadezhda S., from correspondence on the woman.ru forum
You should check with your doctor about the exact frequency of rinsing. Other good anti-inflammatory agents include Rotokan and a solution with hydrogen peroxide - one tablespoon per half glass of water.
Decoctions based on medicinal plants
Self-prepared decoctions from some plants with medicinal properties can help reduce the intensity of symptoms and prevent further spread of inflammation. Such drugs are recommended exclusively as supportive symptomatic therapy, but not as the main treatment. Therefore, before you start using such folk remedies, in any case you need to visit a doctor.
For inflammation of the oral mucosa, the following recipes are usually recommended:
- pharmaceutical chamomile - pour 2 tablespoons of dried flowers with boiled water, cool, strain and use for rinsing,
- calendula - pour a tablespoon of flowers with a glass of boiling water, leave, strain and use the resulting liquid for rinsing,
- sage - to prepare a decoction, you need to brew a tablespoon of flowers in half a liter of water and cool to room temperature,
- yarrow – boil 2 tablespoons of inflorescences for 15 minutes, strain and use for mouth baths.
At home, decoctions of medicinal herbs can be used.
Separately, you can highlight a decoction of oak bark, which has pronounced astringent properties and helps to effectively strengthen soft tissues. To prepare the product, you need to boil a handful of crushed raw materials for half an hour. Cool and strain before use.
Preventive measures
Prevention of gum disease consists of maintaining oral hygiene at home, as well as regular professional cleanings. You need to visit the dentist twice a year, promptly treat dental diseases, replace old fillings and dentures.
One way to prevent gingivitis is to eat a balanced diet. It is important to eat right, choose foods and drinks that are warm or at room temperature. Do not ignore the importance of using dental floss and mouth rinses after every meal.
Dentists at STOMA clinics know how to treat gingivitis: the accumulated experience, advanced diagnostic and therapeutic methods in the arsenal of our specialists allow us to provide urgent dental care to patients and develop effective treatment regimens.