From this article you will learn:
- What is the difference between periodontal disease and periodontitis?
- causes and symptoms of its development,
- how to treat periodontal disease at the dentist, as well as home therapy products.
The article was written by a dentist with more than 19 years of experience.
Periodontal disease is a disease of the gums, which is based on the process of sclerosis of blood vessels, which leads to a decrease in the supply of oxygen and nutrients, and as a result, there is a slow degeneration of all periodontal tissues (i.e., the bone tissue around the tooth, periodontal fibers attaching the tooth to bones, as well as soft tissues of the gums).
Typically, patients incorrectly use the term “periodontal disease” to refer to any existing gum disease. In fact, periodontal disease is a fairly rare disease, and most patients who complain about problems in the gums do not have periodontal disease, but actual chronic generalized periodontitis.
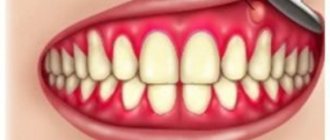
Periodontal disease: photos of teeth and gums
You can very easily check whether you have periodontitis or periodontal disease - the symptoms of the latter are a gradual decrease in the height of the gums and exposure of the roots of the teeth, which occurs due to the gradual process of sclerosis and dystrophy - usually in the absence of any inflammation in the gums. In turn, the presence of bleeding and soreness of the gums when brushing, swelling and redness of the gums indicates the presence of inflammation in the gums, i.e. about Periodontitis.
Etiology
The etiology of periodontal disease has not been fully elucidated. Its occurrence is associated with the influence of exo- and endogenous factors, changes in the reactivity of the body. Exogenous factors include nutritional disorders: deficiency, often relative, of proteins, vitamins, especially A, B, G, D and E, mineral salts (especially calcium and phosphorus), microelements (fluorine, iodine, etc.), excess consumption of carbohydrates and fat Of great importance in the occurrence of P. is the microflora of the oral cavity (see Mouth, oral cavity), enzymes and physiologically active substances of dental plaque (see Teeth) and fluid of the periodontal sulcus, as well as tartar. The emergence and development of P. is largely facilitated by malocclusion (see), especially accompanied by overload or underload of the periodontium, reducing its reserve functionality. Endogenous factors include genetic disorders, shifts in interstitial metabolism and its neurohumoral regulation, disturbances in the body's immunological reactivity, blood circulation, respiration, functional and organic changes in internal organs and other factors that cause a decrease in the resistance of periodontal tissues.
Causes of periodontal disease
Medicine does not name the exact causes of this pathology, since it is largely systemic in nature. These can be various processes in the body that cause resorption of gums and bone tissue. In particular, atherosclerotic circulatory disorders in the maxillary and carotid arteries that supply periodontium can contribute to the development of periodontal disease. Or problems with metabolism, leading to metabolic disorders in the oral mucosa. The hereditary factor is also important.
However, the most common causes of the disease are known:
- bite defects;
- periodontal trauma;
- poor oral hygiene;
- lack of vitamins and minerals in the body;
- low level of immunity;
- endocrine pathologies that lead to disruptions in the production of hormones;
- passion for bad habits;
- neurological problems.
It is noteworthy that tartar, which often forms during periodontal disease, is more a consequence than a cause of the disease.
Pathogenesis
The pathogenesis of periodontal disease is determined by the interaction of general and local factors. At the same time, the above-mentioned exo- and endogenous etiological factors that induce P. (for example, functional disorders of internal organs and systems, oral microflora, dental plaque, etc.) are involved in the mechanism of its development and become pathogenetic.
Most researchers consider immunol disorders, reactivity of periodontal tissues under the influence of dental plaque components, metabolic disorders, inflammation of periodontal tissues (see), microcirculation disorders (see), arising as a result of neurohumoral changes in the body, to be the main ones in P.'s pathogenesis (see). Inflammatory mediators (histamine, serotonin and heparin released from mast cells, kinins - bradykinin, kallidin, prostaglandins, etc.), as well as enzymes of plaque and gingival crevicular fluid and other factors cause irritation and subsequent vegetation of the gingival epithelium deep into the periodontal gap, As a result, the circular ligament of the tooth is destroyed with the formation of a periodontal pocket. The inflammatory process in periodontal tissues is accompanied by symptoms of acidosis and pronounced functional disorders of microcirculation, which leads to degeneration of the bone tissue of the dental alveoli, their resorption and atrophy, loosening and loss of teeth.
A significant role in the pathogenesis of P. is played by functional disorders of microcirculation in periodontal tissues, beginning with a short-term phase of vascular dilation caused by the influence of biologically active substances (kinins, histamine, lysosomal enzymes, prostaglandins, etc.) followed by a long-term spasm (neurogenic genesis) and a decrease in volume blood flow speed. At the same time, the permeability of the vascular wall is disrupted - the initial increase in permeability is replaced by its decrease. The rheological properties of blood are also disrupted with thrombosis of the microvasculature of periodontal tissues. The level of oxygen tension and redox processes in periodontal tissues decreases, which indicates their dystrophy, as a result of which functional changes in blood vessels become organic, having a sclerotic character.
Due to the loss of teeth, pain when chewing, and mobility of teeth, food is not crushed enough, injures the mucous membrane of the mouth, esophagus, and stomach, which, along with a decrease in the secretion of gastric and pancreatic juice, contributes to the development of pathological changes in the gastrointestinal tract. Periodontal pockets, being foci of infection, can lead to sensitization of the body, allergic damage to the heart, kidneys, joints, etc.
Pathological anatomy
Rice.
1-3. Schematic representation of the formation of a periodontal pocket during periodontal disease (according to A. I. Evdokimov). Rice. 1. The relationship between tooth and periodontal tissue in a healthy person: 1—gingival groove (gap); 2 - interalveolar bone septum. Rice. 2. Initial stage of periodontal disease: 1 - periodontal pocket; 2—resorbable interalveolar bone septum; 3 - epithelium that has grown along the root of the tooth. Rice. 3. Severe stage of periodontal disease: 1 - periodontal and bone pocket formed as a result of resorption of the interalveolar bone septum; 2 - remains of the interalveolar bone septum. Periodontal disease usually begins with inflammation of the gums, occurring as chronic, catarrhal gingivitis (see). In the lumen of the gingival sulcus, abundant layers of loose basophilic masses are formed, including colonies of microbes and single epithelial cells. Later, on the basis of a dense supra- and subgingival plaque rich in microbial flora, tartar is formed (see), which aggravates the pathol, periodontal changes. Chronic gingivitis is accompanied by inflammatory infiltration of the gums with lymphoid, plasma cells, swelling of the gums, active proliferation, vegetation in the underlying connective tissue base of the gums, as well as increased desquamation of epithelial cells. The composition of the cellular infiltrate (lymphoid and plasma cells) is characteristic of a delayed-type hypersensitivity reaction. Already at this stage of the disease, mildly expressed lacunar resorption of the alveolar process bone is detected in the periodontal bone tissue (color fig. 1, 2).
The next stage of the pathological process is the formation of a periodontal pocket, characterized by the destruction of the epithelial cover in the area of the periodontal junction, the vegetation of epithelial layers deep into the periodontal gap. Electron microscopy, according to Carson and Sayegh (RE Carson, ES Sayegh, 1978), shows the disappearance of collagen fibrils of the periodontal ligament, which are normally woven into the cement. The contents of the periodontal pocket are necrotic detritus - structureless, basophilic and oxyphilic masses with colonies of microbes and destroyed leukocytes. The outer walls and bottom of the periodontal pocket are formed by granulation tissue, penetrated by branching layers of stratified squamous epithelium. In the bone structures of the alveolar process, pronounced resorptive changes are observed (tsvetn. Fig. 3), starting in the area of the apex of the alveolar process and leading to its complete resorption. Subsequently, resorbtin lacunae containing osteoclasts appear in the underlying sections of the walls of the dental alveoli, which leads to a gradual thinning of the interalveolar bone septa. At the same time, there is a thinning of the spongy bone in the thickness of the interalveolar septa. The resorption process can proceed as smooth resorption, lacunar resorption, and also as oncosis (as a result of bone cells acquiring the ability to osteoclase).
Against the background of patol, changes in the periodontium and as the periodontal pockets deepen in the adjacent areas of the periodontium, progression of hron and the inflammatory process is observed. Its morphological manifestations are the formation of dense lymphomacrophagic infiltrates with an admixture of plasma cells, the formation of fields of granulation tissue, and with exacerbation patol. process - solitary, and in some cases - multiple abscesses. With the progression of periodontal disease, periodontal pockets and the submersible growth of layers of stratified squamous epithelium, which are reactive in nature, reach the apexes of the roots of the teeth, and the periodontal ligament is completely destroyed. Further resorption of the bone tissue of the alveolar process leads to complete resorption of the interalveolar and interradicular bone septa (tsvetn. Fig. 3). With P., tooth tissue is involved in the pathological process quite early: cement resorption begins, which leads to the formation of deep cement and cemento-dentin niches. In parallel, the process of new formation of cement can be observed. If this process predominates, hypercementosis develops. In the pulp of teeth during P., dystrophic changes expressed to varying degrees are found, leading to its reticular atrophy, as well as to the formation of single and multiple petrificates and denticles in the pulp. Often with P., the development of retrograde pulpitis is noted, which can result in the death of the pulp.
Rice. 1. Histotopogram of the lower jaw with periodontal disease: 1 - teeth; 2 - Interalveolar bone septa with preserved contours of the apexes; 3 - areas of osteosclerosis; 4 - areas of osteoporosis; hematoxylin-eosin staining; x3. Rice. 2. Microspecimen of jaw bone tissue for periodontal disease: 1 - bone plates; 2 - artery with thickened walls and narrowed lumen; 3 — obliteration of the lumen of the vessel; hematoxylin-eosin staining; x 200.
Periodontal disease can occur with the predominant development of dystrophic changes in the periodontal tissues with characteristic atrophy of the bone trabeculae of the spongy substance, pronounced focal osteosclerosis, alternating with focal osteoporosis (Fig. 1). Patol, changes in bone tissue are combined with pronounced changes in its blood vessels: hyperplasia of the inner membrane, sclerosis and hyalinosis of the middle membrane, sharp narrowing or complete obliteration of the lumen of the vessels (Fig. 2).
In the connective tissue base of the gums, pronounced changes in blood vessels are also observed, manifested by proliferation of the endothelium, the formation of parietal thrombi, and sometimes the development of vasculitis; Against this background, swelling of collagen fibers, their fragmentation and even lysis are quite often observed. In general, the condition of the gums is characterized by the development of a sluggish inflammatory process in it; in the connective tissue stroma of the gums, an infiltrate of plasma and lymphoid cells is found, localized mainly in the area of the gingival sulcus.
Morfol, changes in the periodontium, similar to those with P. in humans, were obtained in experiments on animals.
Clinical picture
The following stages of P. are distinguished: initial, developed and stage of stabilization (remission). P. usually does not appear immediately in the area of all teeth, but symmetry of the lesion is often observed. However, gradually the process becomes generalized and affects the entire periodontium.
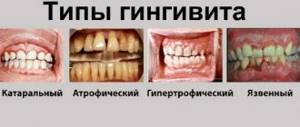
In the initial stage, P. occurs as gingivitis (usually catarrhal and hypertrophic, less often atrophic and desquamative). Bleeding gums, pain or a feeling of itching during eating and brushing teeth, anemia or hypertrophy of the gingival papillae of the tooth, burning or a feeling of numbness in the gums are noted, in most cases there is deposition of supra- and subgingival tartar.
Rice. 3. The appearance of teeth with periodontal disease: the teeth are displaced and rotated along the axis, their roots are exposed.
The developed stage of P., as a rule, is characterized by the presence of generalized gingivitis, pasty gums with symptoms of congestive hyperemia, their bleeding, the presence of periodontal pockets 5-6 mm deep or more, in most cases with the release of pus from them. There is an abundant deposition of dense subgingival calculus, which, unlike supragingival calculus, penetrates deep into the periodontal pockets in the form of thin granular layers, tightly attached to the roots of the teeth. The teeth become mobile, often shift, rotate along an axis (Fig. 3), and fall out. Free spaces form between teeth that were previously in close contact (see Diastema, Trema). Moving teeth injure surrounding tissues and increase inflammation. When the necks and roots of the teeth are exposed, their exposed areas are subject to prolonged irritation when eating, inhaling cooled air, talking, and become a source of pain. Displacement of teeth, impaired diction are noted, and some patients develop bad breath. The general condition, as a rule, suffers slightly, sometimes there is a low-grade fever. But in some cases the condition of patients worsens sharply.
The stage of stabilization (remission) occurs mainly after complex treatment. It is characterized by a subsidence of the inflammatory process and a decrease in tooth mobility, a decrease in the depth of periodontal pockets or their elimination, which occurs, for example, after surgical treatment of P.
In addition to P., which occurs in accordance with the described stages, P. occurs with a predominance of dystrophic changes, which proceeds slowly, without a tendency to exacerbation. At the same time, due to the uniform loss of bone and gum atrophy, periodontal pockets do not form, the teeth remain stable even in the case of significant atrophy of the bone of the alveolar processes. Patients complain of a feeling of itching and numbness in the gums, pain in the exposed necks of the teeth or in the area of wedge-shaped defects in the teeth. P. can be complicated by periodontitis (see), periostitis (see), inflammation of regional lymph nodes (see Lymphadenitis), ascending pulpitis (see), osteomyelitis of the jaws (see), phlegmon of the perimaxillary spaces and neck.
Diagnosis
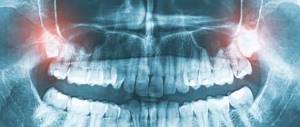
The diagnosis is established on the basis of patient complaints, wedges, pictures, data from radiological, laboratory and functional research methods.
Rice. 4. Panoramic radiograph of the lower jaw with periodontal disease: resorbing interalveolar bone septa, having a characteristic “eaten away” appearance (indicated by arrows).
Roentgenol, P.’s picture depends on the stage of the process. In the initial stage, osteoporosis (see) and destruction of the cortical substance of the apices of the interalveolar septa are detected. In the developed stage, truncation of the apices of the interalveolar septa is noted; along with horizontal resorption, vertical resorption also appears, often with the formation of bone pockets. The contours of the alveolar processes have a characteristic scalloped, “eaten” appearance (Fig. 4), and the deposition of subgingival tartar is determined. The increase in patol, the process is manifested by the appearance of foci of spotted osteoporosis and the formation of bone abscesses. The stabilization stage is radiographically manifested by compaction of the contours of the ridges of the interalveolar septa and the disappearance of foci of spotty osteoporosis.
Rice. 5. Panoramic radiograph of the lower jaw with periodontal disease: 1 - uniformly reduced interalveolar bone septa; 2 - foci of osteoporosis; 3 - focus of osteosclerosis; 4 - narrowed periodontal fissures; 5 - tartar.
The X-ray picture of periodontal disease with a predominance of dystrophic changes in the periodontium is characterized by a uniform decrease in the height of the interalveolar bone septa, sclerosis of the bone tissue of the alveolar process, and narrowing of the periodontal gap (Fig. 5).
Wedge, assessment of the periodontal condition is carried out on the basis of bone loss of the alveolar processes, the presence and intensity of inflammation in the tissues of the gingival margin and is expressed in the form of special periodontal indices. The degree of hygienic condition of the oral cavity is determined using colorimetric tests.
Differential diagnosis
carried out with eosinophilic granuloma, Lefebvre-Papillon syndrome, mobility of individual teeth against the background of their long-term trauma by antagonist teeth in case of occlusion. If there is an eosinophilic granuloma in the alveolar process (see) rentgenol, the picture is characterized by diffuse resolution of the bone, extending beyond the periodontal tissues. With Lefebvre-Papillon syndrome rentgenol, the picture is similar to that of the developed stage of P., however, palmoplantar keratosis is characteristic of this syndrome (see Lefebvre-Papillon syndrome). In the case of traumatic occlusion, the diagnosis is clarified by comparison with an x-ray of the teeth of the opposite side.
Symptoms of periodontal disease
The danger of this disease is that it begins asymptomatically, and the patient notices its appearance only when there is a noticeable decrease in the volume of tissue around the tooth. Often the pathological process is hidden by tartar, tightly adjacent to the necks of the teeth, and the diagnosis becomes obvious only after their removal.
The extent of symptoms depends on the stage of the disease. In general, the obvious signs of periodontal disease are:
- exposure of the tooth neck and roots;
- pale gums;
- increased sensitivity of teeth to cold, hot, salty;
- defects in tooth enamel and changes in its color;
- sclerosis of bone tissue (especially noticeable on x-rays);
- visual increase in interdental spaces;
- itching in the gum area;
- loosening of teeth.
Let us note that periodontal disease is generally not characterized by bleeding gums, inflammatory processes and the formation of gum pockets, although these symptoms are not excluded at a late stage.
Treatment
P.'s treatment should be comprehensive, as individualized and systematic as possible. Complex to treat activities include local and general effects on patol, the process in periodontium.
Local treatment involves the elimination of local periodontal factors, removal of supra- and subgingival dental plaque, anti-inflammatory treatment and curettage of periodontal pockets, increasing the activity (or correction) of blood circulation in the periodontium and increasing the reactivity of its structures. Orthopedic treatment of P. is widely used—selective grinding of teeth, splinting, and clasp prosthetics. For the treatment of the initial stages of P., the use of ion-exchange membranes containing various microelements and biologically active substances is effective. In the treatment of periodontal pockets, antiseptics (hydrogen peroxide, thiobiargen solution, ethacridine lactate, iodinol, dimexide, etc.), enzymes (trypsin, chymotrypsin, hygrolithin, ribonuclease), glucocorticoids (hydrocortisone, prednisolone, dexazone, etc.), drugs are used. medicinal herbs (salvin, romazulan, carotolin, chlorophyllipt, etc.), antitrichomonas drugs (metronidazole, fasigin, etc.), protein anabolizers (methyluracil, pentoxyl). Treatment of periodontal pockets is carried out by rinsing with a syringe, instillations and medicinal gum bandages. When radically treating periodontal pockets in order to remove tartar, granulations, as well as deep-growing epithelium, deep curettage is performed - curettage according to Znamensky and Younger-Sachs using a periodontal set or special instruments. Sometimes cryo- and vacuum curettage are used using special devices. In some cases, they resort to gingivectomy or gingivotomy (excision or dissection of a section of the gum) according to the depth of the periodontal pockets or the so-called. patchwork operations. One of them is the Widmann-Neumann-Cieszynski operation, during which a mucoperiosteal flap is cut out from the vestibular side of the alveolar process in the area of four-six teeth and the affected periodontal tissue is exposed. This makes it possible to radically remove granulations and tartar. The mucoperiosteal flap is then placed in place and secured with sutures. However, after this operation there is significant exposure of the necks and roots of the teeth, which limits the indications for it. Favorable results are obtained from operations using allo- and explants. In order to eliminate hyperesthesia of the necks of teeth, fluoride varnish, applications of 10% calcium gluconate solution, 1 - 2% sodium fluoride solution, fluoride paste, etc. are used, and physiotherapeutic methods of treatment are also used.
General treatment is aimed at eliminating inflammatory changes in the periodontium, hyposensitization of the body, increasing the reactivity of the body and periodontium, preventing lesions (primarily microcirculatory) periodontal vessels, as well as treating common concomitant P. diseases. In order to reduce the intensity of inflammation in the periodontium in cases of severe process, broad-spectrum antibiotics (lincomycin, oleflavit, rondomycin), sulfonamides (biseptol) are used in the pre- and postoperative periods. To hyposensitize the body, diazolin, pipolfen, calcium chloride, and tavegil are used. Fluorine preparations, prodigiosan, ATP, trental, venoruton, antioxidants, adaitogens, etc. are used as agents for pathogenetic therapy. In the presence of diseases aggravating the course of P. (diabetes mellitus and other endocrine diseases, diseases of the gastrointestinal tract, cardiovascular systems), treatment of P. itself is combined with treatment of the disease aggravating the course of P.
Physiotherapeutic treatment is most effective in the initial stage of P. When using these methods, blood circulation and trophism of periodontal tissues improve. Physiotherapy is carried out using electro- and phonophoresis of heparin, antioxidants (dibunol, galascorbine, vitamin E), prostaglandin inhibitors (aspirin, indomethacin, ATP, trental). Hydro-, electro- and vibration therapy are used to treat periodontal disease, and hydrotherapy usually precedes other treatment methods. Electrophoresis of vitamins B1, C, etc. is carried out (see Electrophoresis). The use of pulse currents (see) - diadynamic, fluctuating and sinusoidal modulated currents - is important. Darsonvalization (see) and helium-neon laser are also used. Laser therapy (see Laser) reduces inflammation, normalizes blood circulation in periodontal tissues, and stimulates metabolic and regeneration processes. After curettage, local ultraviolet irradiation is indicated, which reduces tissue swelling and improves epithelization of the wound surface. Usually after 2 weeks. After surgical interventions, calcium or fluoride electrophoresis is prescribed. It is advisable to use resort factors (balneotherapy and peloid therapy).
In case of tooth mobility, secondary traumatic occlusion and purulent discharge from periodontal pockets, electrotherapy and massage are contraindicated; Hydrotherapy with the addition of medications is recommended.
How to treat periodontal disease -
If you have been diagnosed with periodontal disease, the symptoms and treatment will be interrelated, etc. This disease is based on the phenomena of vascular sclerosis and bone tissue degeneration - the main methods of treatment will be physiotherapy and drug therapy, aimed primarily at stimulating blood circulation in the gums. In addition, selective grinding of the contacts between the lower and upper teeth is carried out, and at the first symptoms of mobility, teeth are splinted with crowns or fiberglass.
Treatment of periodontal disease at home is limited only to the use of finger massage of the gums, the use of special gels for the gums and toothpastes, as well as the ingestion of various vitamins, antioxidants and some other drugs (we will discuss them below). All other treatment will involve professional dental care in a physiotherapy office.
Finger massage of gums –
Finger massage of the gums for periodontal disease is carried out every day, in the morning after brushing your teeth. The direction of movement of the fingers should coincide with the direction of lymph flow in this area, i.e. you should make circular massaging movements, which should gradually move from the front teeth - towards the chewing teeth. The procedure time is 3-5 minutes for each jaw. In addition to this massage, you can periodically (several times a year) conduct physiotherapy courses.
The massage can be done without everything, or using one of the special gels that additionally stimulate blood circulation in the gums. For example, this could be the drug Asepta in the form of a gel, which contains propolis (a beekeeping product). This gel can also be used without massage, simply applying it to the gum margin after brushing your teeth in the morning and evening. However, it should be noted that you will not be able to cure periodontal disease at home only with finger massage and gum gel.
An important point is that gum massage cannot be performed against the background of gum inflammation (with swelling, redness or severe cyanosis of the gums, as well as in the presence of deep periodontal pockets and subgingival dental plaque). Otherwise, an intensification of the inflammatory reaction and the development of purulent abscesses in the projection of periodontal pockets is possible.
Physiotherapy for periodontal disease –
There is a large list of physiotherapeutic methods for treating gum periodontal disease - these are electrophoresis, phonophoresis, vacuum massage, vibration vacuum massage, magnetic therapy, diadynamic currents, laser therapy. The problem is that not even every dental clinic has its own physiotherapy department, and residents of large cities are luckier here (especially where there are university dental clinics at medical universities).
For example, in Moscow there is a large department of physiotherapy for periodontal diseases at the state clinic TsNIIS (Central Research Institute of Dentistry). You can get a referral for physical therapy from your dentist. Next, we will talk in detail about some of the main physiotherapeutic techniques that are used for periodontal disease...
- Electrophoresis and phonophoresis of heparin - heparin has a significant therapeutic effect in periodontal disease, because
it has the ability to reduce tissue hypoxia, normalizing the oxygen balance of tissues, microcirculation and transport of substances between blood and tissues. Heparin electrophoresis is carried out according to the usual method: make gauze pads from a sterile bandage under each electrode, soak each pad - first with 1.0 ml of distilled water, then from a syringe - 1 ml of heparin solution. The concentration of heparin in 1.0 ml of solution should be 5000 units. Electrodes with gauze pads are placed on the gingival edge of the alveolar process of the jaws, while the electrodes are carefully isolated from saliva with cotton rolls. Heparin is always administered from the cathode only. The duration of the procedure is from 12 to 15 minutes. The course of treatment is 10-12 procedures (in a row, daily). In addition, heparin can be successfully introduced into periodontal tissue not only by electrophoresis, but also using the phonophoresis technique on the Ultrasound T-5 apparatus. The duration of the phonophoresis procedure is about 7-10 minutes.
- Vacuum massage - this method is tens and hundreds of times more effective than regular gum massage, which you can do at home.
Vacuum massage is carried out using a special Kulazhenko vacuum apparatus or similar devices in a physiotherapy room. This massage leads to the destruction of part of the capillaries, which is accompanied by the release of histamine, which tends to stimulate blood circulation. Even more effective is the creation of vacuum hematomas along the transitional fold during vacuum massage of the gums. For this, the pressure is set to 1 atmosphere, and the nozzle of the device must be held in one place for 30 to 60 seconds - until a hematoma of 4-5 mm in size is formed. During one visit, you can do no more than 5-6 such hematomas (a full course - 8-12 procedures, with breaks between procedures - 3-5 days). This method further stimulates metabolic processes and blood supply to the gums.
- The use of a laser - the use of a helium-neon laser for periodontal disease is aimed at enhancing tissue trophism, metabolic processes, and blood circulation. The course of treatment is usually 12-15 sessions, and is carried out several times a year. A single laser exposure should not exceed 20 minutes.
Drug therapy for periodontal disease –
There are several groups of drugs that can be effective in increasing blood circulation and reducing hypoxia in periodontal tissues.
These may be antioxidants, anabolic steroids, the use of certain vascular drugs that stimulate peripheral circulation. 1) The use of antioxidants - clinical studies have shown that sclerosis of blood vessels in periodontal tissues leads to a significant decrease in oxygen delivery to the gums and the development of hypoxia, which triggers the process of sclerosis of bone tissue. Therefore, a number of drugs to stimulate oxygenation can be very useful. These drugs include substances with antioxidant properties. First of all, this can be vitamin E, as well as vitamins A, C, P and group B.
2) The use of anabolic steroids - the use of this group of drugs is justified primarily in men, because drugs have an androgenic effect. In women, this may result in a deepening of the voice and menstrual irregularities, which disappears only with discontinuation of the drug. In addition, the prescription of this group of drugs should always be preceded by a consultation with a therapist and endocrinologist regarding the absence of contraindications. The drug "Retabolil" is prescribed at a dose of 25-30 mg IM, only once every 3 weeks (the full course of treatment is about 5-7 injections).
3) The use of Trental - the possibilities of increasing blood circulation in periodontal tissues are limited by the limits of the ability of blood vessels to expand, and with significant sclerotic changes in blood vessels in periodontal tissues - physiotherapeutic effects on the gums alone are no longer enough. In this regard, in case of moderate to severe periodontal disease, it also makes sense to prescribe drugs for the treatment of blood microcirculation disorders.
For these purposes, the drug Trental can be used. This drug contains pentoxifylline, which increases the concentration of amino monophosphate in the smooth muscle of the vascular wall (by inhibiting the enzyme phosphodiesterase). An increase in the concentration of amino monophosphate in the membranes of smooth muscle cells helps to reduce the contraction of the smooth muscles of the vascular wall, thereby increasing the lumen of the capillaries.
Trental also affects the rheological properties of blood - in particular, it increases the elasticity of red blood cells. Blood capillaries in the area of interdental gingival papillae and periodontal tissue have a very small lumen, and therefore disturbances in the elasticity of red blood cells can lead to disruption of tissue trophism (i.e., their saturation with oxygen and nutrients). In addition, trental additionally inhibits erythrocyte aggregation, thereby preventing microvascular thrombosis, which is often observed in periodontal disease.
Prescription regimens: the drug is prescribed 2 tablets of 100 mg each - 3 times a day (16 days in total), after which the drug is taken 1 tablet of 100 mg - 3 times a day for another 1 month. However, the combined use of trental is even more effective. The combination includes a course of administering trental by electrophoresis (from the cathode) or by phonophoresis + oral administration of the drug according to the scheme indicated above.
Selective grinding of teeth –
When treating periodontal disease, it is very important to take into account that in such patients there is an excess of calcium in the hard tissues of the teeth, which leads to a delay in the physiological wear of the teeth. This would seem good, but in fact it leads to the formation of a traumatic bite in the area of the front teeth and their gradual fan-shaped divergence. Therefore, it is very important to send the patient to an orthopedic dentist for selective teeth grinding - in order to normalize the contacts between the upper and lower teeth.
In addition, delayed abrasion of the cusps on the chewing surfaces of the teeth, leading to the development of a traumatic bite in the area of the anterior teeth, can cause not only their fan-shaped divergence, but also the formation of a large number of wedge-shaped dental defects.
Splinting of mobile teeth –
The procedure for splinting teeth can be performed with fiberglass or artificial crowns, the need to choose between which will be dictated by the clinical situation in the oral cavity. Indications for the use of this method will be the emerging mobility of teeth, or their fan-shaped divergence (consisting in the displacement of teeth and an increase in interdental spaces). Read more about this method using the link above.
Use of toothpastes and gels –
Toothpastes and rinses from the Mexidol-Dent series are especially suitable for increasing blood circulation in the gums. They contain an antioxidant that helps reduce the level of hypoxia in periodontal tissues, which inevitably occurs due to hardening of blood vessels during periodontal disease. Toothpastes based on propolis can also have a stimulating effect on the blood supply to the gums (24stoma.ru).
Prognosis and Prevention
Forecast.
Treatment carried out according to indications slows down or stops the process. As a result of rational comprehensive treatment of periodontal disease, recovery with residual effects (relief) and stable recovery (stabilization of the process) can occur. Untimely treatment and irrational use of pathogenetic therapy lead to the gradual loss of several or all teeth.
P.'s prevention is carried out with mandatory consideration of professional characteristics, climatic and geographical conditions and concomitant diseases. Complex prevention includes clinical examination of patients, which is aimed at identifying the initial stages of P.; carrying out preventive measures, organizing specialized periodontal centers, departments and offices.
Primary preventive measures are aimed at developing hygienic skills, timely treatment of inflammatory changes in the tissues of the gingival margin, regular removal of dental plaque, treatment of dentition anomalies, and rational orthopedic treatment.
The complex of secondary preventive measures includes the elimination of early signs of pathol, changes in the oral cavity - monitoring its hygienic condition, eliminating factors that contribute to the retention of food accumulations in the interdental spaces, and preventing dental caries. Therapeutic, surgical and orthopedic measures aimed at eliminating pathol, the process, preventing complications and restoring the function of the masticatory apparatus are carried out both for therapeutic purposes and to prevent the progression of the process and its complications. They use means and methods aimed at stimulating microcirculation and trophism of periodontal tissues using physiotherapeutic methods, finger massage, rinsing the mouth with water at a contrasting temperature, as well as removing dental plaque. According to indications, surgical relocation of the frenulum and formation of the vestibule, elimination of primary traumatic contacts between teeth using selective functional grinding of the cusps, elimination and replacement of incorrectly made fillings and dentures, treatment of bruxism (see) and dentoalveolar anomalies are carried out.
The scheme of preventive recommendations should include a fractional balanced diet with a sufficient amount of fresh vegetables and fruits, vegetable oils, lactic acid products and others.
Bibliography:
Evdokimov A.I. On the issue of pathological anatomy, etiology and pathogenesis of periodontal disease (periodontal disease), Dentistry, No. 6, p. 10, 1939; Evdokimov A.I. and Nikitina T.V. Criteria for the curability of periodontal disease, ibid., t. 56, No. 5, p. 14, 1977; Shizhina N. A. and Prokhonchukov A. A. The role of disorders of the functions of internal organs and body systems as common background factors in the pathogenesis of periodontopathies, M., 1971; Ivanov V. S. Periodontal diseases, M., 1981; Kabakov V.D. and Belchikov E.V. Issues of immunology of periodontal disease, L., 1972; Kodola N.A., Khomutovsky O.A. and Tsentilo T.D. Periodontal disease, ultrastructure of the gums and pulp, Kyiv, 1980; Kopeikin V. N. Orthopedic treatment of periodontal diseases, M., 1977; Lemetskaya T. I. Periodontal diseases (periodontopathies), M., 1972; Novik I. O. Periodontal disease (pathogenesis, clinic, treatment), Kyiv, 1964; Platonov E. E. Tasks and ways of studying periodontopathies, Dentistry, No. 5, p. 3, 1964; Prokhonchukov A. A. and Zhizhina N. A. Pathogenesis of experimental periodontopathies, M., 1971; Guide to therapeutic dentistry, ed. A. I. Evdokimova and A. I. Rybakova, M., 1967; Rybakov A.I. and Ivanov V.S. Clinic of therapeutic dentistry, p. 192, M., 1980; Proceedings of the 6th All-Union Congress of Dentists, M., 1976; Experimental and clinical dentistry, ed. V. V. Panikarovsky, M., 1978; Experimental and clinical dentistry, ed. A. I. Rybakova, vol. 4, p. 89, 98, M., 1973; Epidemiology, etiology and prevention of periodontal diseases, Report of the WHO scientific group, M., 1980; Bernard R. D. La ionoforesi, Dent. Cadm. (Milano), v. 46, no. 10, p. 49, 1978; Carson RE, Sayegh FS a. Fedi PF Osteoclastic resorption of alveolar bone affected by periodontitis - correlation of light microscopic and scanning electron microscopic observations, J. Periodont., v. 49, p. 406, 1978; Glickmanl. Clinical periodontology, Philadelphia, 1979; Goldman H. M. a. Cohe n DW Periodontal therapy, St Louis, 1973; K 6-tzschkeH. Leitfaden der Parodontologie, Lpz., 1969; Kostlan J. a. Skash M., Onemocneni parodontu, Praha, 1967; Page RCa SchroederH.E. Pathogenesis of inflammatory periodontal diseases, Lab. Invest., v. 34, p. 235, 1976; Physikalische Therapie in der Stomatologie, hrsg. v. K. Jarmer, B., 1960; Waernaug J. Subgingival plague and loss of attachment in periodontosis as observed in autopsy material, J. Periodont., v. 47, p. 636, 1976.
V. S. Ivanov, T. I. Lemetskaya, T. V. Nikitina; R. I. Mikhailova (physiot.), V. V. Panikarovsky (pathological an.), A. A. Prokhonchukov (etiol., pathology).
Periodontal disease - history and causes of the disease
It is a mistake to think that periodontal disease is a disease of the modern age, and our ancestors had never heard of it. People have suffered from periodontal disease at all times. And believe me, it was much more difficult for our predecessors, because due to the low level of development of medicine, this disease mercilessly deprived people of their teeth. Fortunately, today is the 21st century, and tooth-preserving technologies are a priority in dentistry. Therefore, at the first signs of the disease, the doctor and the patient take a whole range of measures to preserve a full set of 32 teeth in the oral cavity.
Where to look for the causes and origins of periodontal disease? In the old days, according to experts, the main prerequisite for the development of periodontal disease was a monotonous diet and an unbalanced diet. Perhaps this is really so, and you can judge this at least from a book of recipes from past centuries. So, our ancestors ate mainly meat and fish dishes, but finding some kind of salad recipe was an extremely difficult task; such dishes were unheard of then. This naturally suggests the conclusion that people suffered from a lack of vitamins, a deficiency of microelements, and one of the consequences was the development of periodontal disease. By the way, many of our contemporaries suffer from the disease for the same reason, that is, an unbalanced diet and the habit of monotonous food.
The second common reason is insufficient load on the gums. If you want to protect yourself from periodontal disease, be sure to eat fresh vegetables and fruits. They will not only serve as a source of vitamins and microelements for the whole body, but will also be a simulator for teeth and gums if you regularly gnaw on apples, carrots, pears, etc. This kind of massage will ensure high-quality blood supply to the gum tissue, which is an excellent preventative measure periodontal disease.
However, periodontal disease in modern inhabitants of the planet, as practice shows, is most often due to another reason. The disease develops under the influence of dental plaque, which turns into tartar. The latter, remaining on the teeth, gradually does its dirty work - it injures the gums, the tissues that surround the tooth, and therefore contributes to the development of the inflammatory process. Illegally installed fillings and crowns “work” in exactly the same way. They also undermine the health of the gums, as they put pressure on them, and the result is inevitable inflammation.
It injures the gums and causes periodontal disease, as well as crowded teeth and bite defects. The fact is that it is very difficult to efficiently clean such teeth from plaque, which means that it constantly accumulates on the teeth, forming an excellent habitat for the life and reproduction of pathogenic bacteria. Having settled in the oral cavity, they cause inflammation and destroy tissue, and this process will actively continue until high-quality hygiene rids the teeth and gums of pests. Moreover, it is important not only to clean your teeth daily using your usual toothpaste and brush, but also to have regular professional cleaning, which will reliably rid your teeth of plaque and tartar.
But these are not all the reasons why periodontal disease overtakes a person. In particular, the patient may be genetically predisposed to the disease, so it is worth paying attention to the dental health of your parents and grandparents. In addition, periodontal disease is provoked by common diseases, for example, diabetes mellitus, diseases of the endocrine, cardiovascular systems, gastrointestinal tract and others. The likelihood of periodontal disease increases significantly as soon as a failure in metabolic processes occurs in the body. How to protect yourself and save your teeth? The best way is to undergo a preventive examination with a dentist twice a year, who will recognize the disease at an early stage and can prevent its development, preserving your beautiful smile.